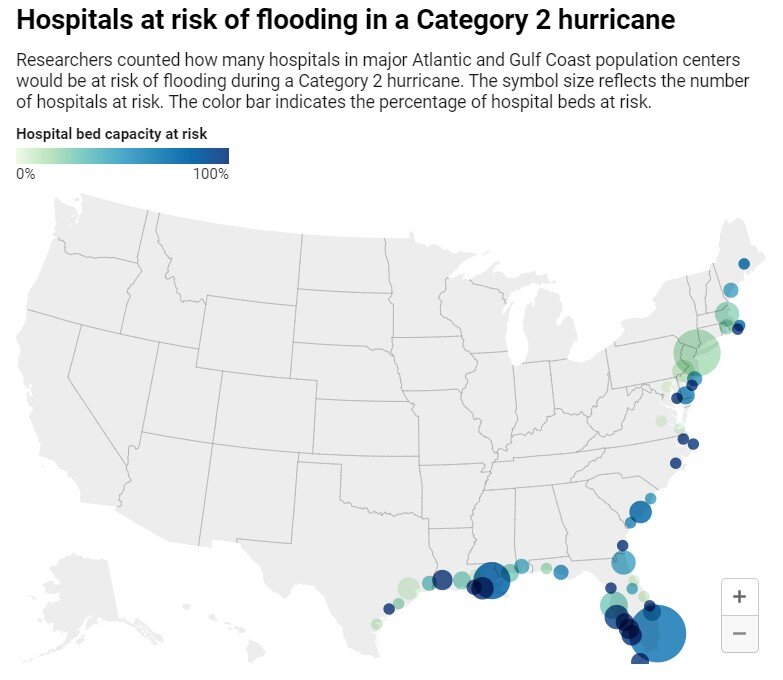
Map: The Conversation/CC-BY-ND Source: Tarabochia-Gast et al., GeoHealth, 2022
Hurricane Ian, one of the most powerful storms to hit the United States, tore off part of the roof from a hospital in Port Charlotte, Florida, and flooded the emergency room on the lower level of the building, leaving staff trying to move patients as water poured inside. nine hospitals and dozens of nursing homes had to transfer the sick after loss of access to clean water because of the storm.
Health services are important at all times, but when disasters strike, these services become even more important when the number of injuries increases.
However, in many coastal communities, hospitals have been built in places that are at increased risk of flooding during hurricanes.
I am studying ways to improve disaster communicationsincluding how health care organizations prepare for severe weather events. Here’s what the study says about rising risks.
A high percentage of coastal hospitals are at risk
Given the effects of climate change, many areas are vulnerable to severe weather events and hazards. Medical facilities, including hospitals, clinics and long-term care facilitiesare no exception.
A study released on September 29, 2022, as Ian left Florida, found that even weak hurricanes can cause a serious risk to many hospitals along the coast of the United States.
At 25 metropolitan areas along the Atlantic and Gulf coasts, the authors found that at least half of hospitals are at risk of flooding in a Category 2 storm, defined as winds between 96 and 110 miles per hour. In some cities, including Lake Charles, Louisiana; In Naples, Florida and Ocean City, New Jersey, 100% of hospitals are considered at risk.
These risks are increasing with climate change. The authors of the Harvard University study estimated that 22% chance of coastal hospitals being flooded of this century.
What is important about this finding is that communities can begin to identify high-risk hospitals and develop both backup plans and measures to help protect them and their patients.
The US has its own history hospital disasters during severe weather conditions. Aftermath of Hurricane Katrina in 2005 opened many eyes to what broken healthcare systems look like. during that storm many hospitals were without electricity and the ability to communicate, as well as damaged water and sewer services. Several of them were unable to replenish their supplies of food, medicine, blood and linen, but had to continue operations in terrible conditions.
TV Drama”Five days in memory” is based on that disaster and how the staff at New Orleans Memorial Medical Center struggled to keep patients cut off by floodwaters alive. It sparked a lot of conversation about preparedness and risk at these critical facilities.
Elderly communities are being ignored
My research examines how disadvantaged and vulnerable populations prepare for and cope with disasters. In particular, I conducted fieldwork analyzing how older people live in retirement and retirement communities be aware of your own risks.
Photos from a friend in Tampa showing how Tampa General Hospital is preparing for Hurricane Jan. The hospital is being surrounded by a temporary flood barrier, the likes of which I have never seen before. Interesting construction. There is a high chance of flooding due to the storm. #k5weather pic.twitter.com/wgPbtATtsh
— Rich Marriott (@rtmarriott) September 27, 2022
Ideally, these facilities should be able to provide the same services during disasters as before without interruption. The reality is that when the infrastructure is overloaded, the elderly may find themselves in dangerous conditions and unable to evacuate. They may also not be mobile enough to be easily rescued, especially if the facility spans multiple floors.
Staff may not be available to administer medication. Electricity or energy for life-sustaining medical treatment may not be available. Medical workers in these institutions nor is it always possible to implement disaster plans or protocolsif there are such plans.
After Hurricane Irma knocked out power in Florida in 2017, a dozen patients died at a nursing home where the power to the air conditioning went out. This led to the state law that now stands requires nursing homes to have backup generators. But Ian showed that even this is not enough for the safety of the residents.
Other populations such as people with physical, sensory or cognitive disabilities, and those who are medically vulnerable, including the homeless, also need to be considered in health care-related disasters. While the homeless can find shelters, including those created for disaster relief, it is not uncommon for homeless people to seek medical care or seek refuge in hospitals.
Resilience and disaster plans
After disasters, hospitals are needed for treatment injury growthand mental health issues among disaster victims. More than 700 rescues were launched during and after John.
It is therefore important that hospitals, like nursing homes, develop hospital disaster resilience plans. These plans for hospitals cover topics such as safety, staffing, increasing capacity to handle sudden increases in patient numbers, emergency services during flooding, and disaster plans, training and communications.
In the long run, better building design, flood barriers and more secure locations may be required.
The Southeast Louisiana Veterans Health Center in New Orleans is one model for how to design a medical facility to withstand a disaster. The building was built to handle high winds, and the emergency room is on the second floor, at least 21 feet above the base flood elevation.
Just received this video from Fawcett Memorial Hospital in Port Charlotte. I spoke to two people who work here and they said part of the roof on the 4th floor is off. This floor is intensive care #abc11 #Hurricane_John pic.twitter.com/dgnJgbK3ID
— Josh Chapin (@JoshChapinABC11) September 28, 2022
Storms like Ian are a stark reminder of the importance of protecting these facilities so that emergency medical care is available in the event of a natural disaster, and why disaster planning is critical in all health care settings.
Provided
Conversation
This article is reprinted from Conversation under a Creative Commons license. To read original article.![]()
Citation: Hurricane Ian Shows Increased Risk of Severe Storms for Medical Facilities (2022, October 3) Retrieved October 3, 2022, from https://medicalxpress.com/news/2022-10-hurricane-ian-severe-storms- health.html
This document is subject to copyright. Except in good faith for the purpose of private study or research, no part may be reproduced without written permission. The content is provided for informational purposes only.