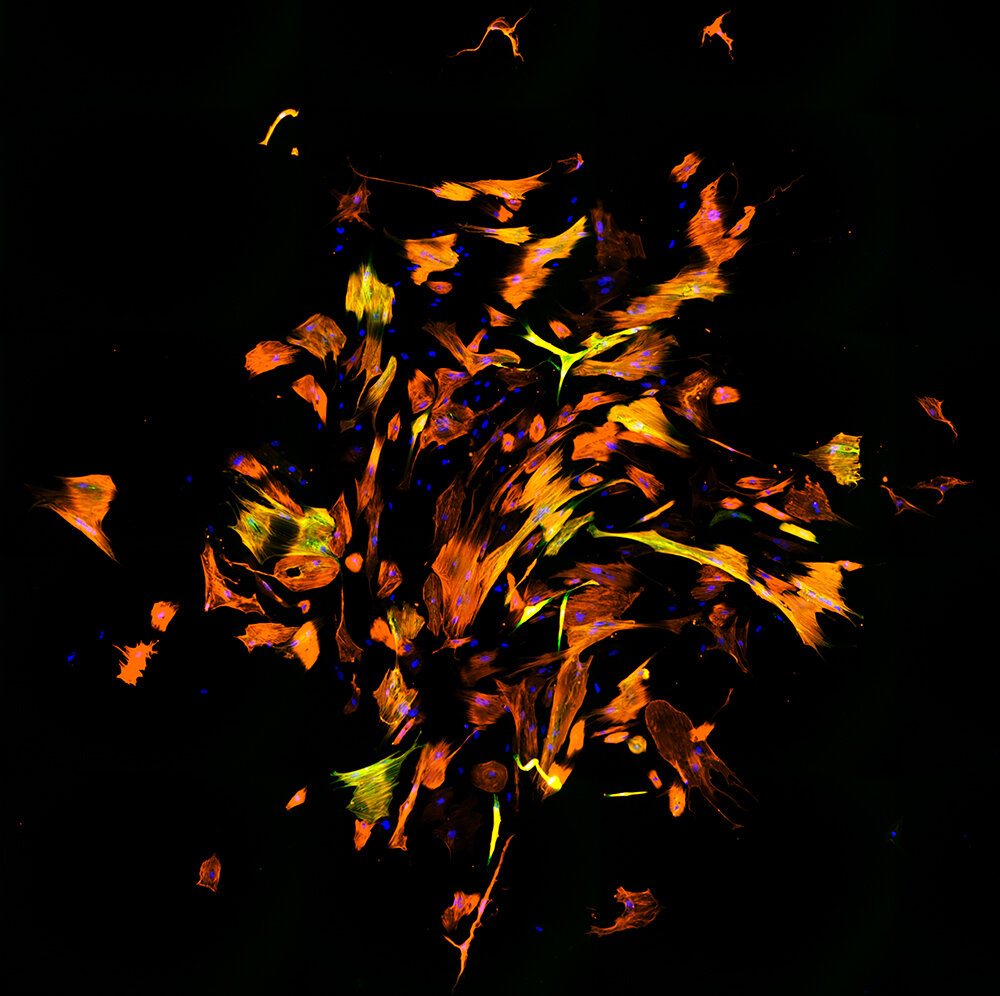
Reprogram human fibroblasts into cardiomyocyte-like cells. Immunofluorescence shows different molecules: DNA (blue), cardiac troponin T (orange), and α-actinin (green). Credit: Qian Lab, UNC School of Medicine
Scientists at the UNC School of Medicine have made significant progress in the promising field of cell reprogramming and organ regeneration, and the discovery could play an important role in future drugs to treat damaged hearts.
In a study published in the journal Cellular stem cellscientists from the University of North Carolina at Chapel Hill discovered a more streamlined and efficient method reprogramming scar tissue cells (fibroblasts) to become healthy heart muscle cells (cardiomyocytes). Fibroblasts produce fibrous, stiff tissue that contributes to heart failure after or because of a heart attack heart disease. The transformation of fibroblasts into cardiomyocytes is being investigated as a potential future strategy for treating, or even someday curing, this common and deadly condition.
Surprisingly, the key to the new technique for creating cardiomyocytes turned out to be a protein that controls the activity of a gene called Ascl1, which is known to be an important protein involved in the transformation of fibroblasts into neurons. The researchers believed that Ascl1 was specific for neurons.
“This is an unusual finding, and we expect it will be useful for the development of future cardiac treatments and possibly other types of therapeutic cellular reprogramming,” said senior study author Li Tian, Ph.D., associate professor of pathology and laboratory medicine at UNC and vice director of the McAllister Heart Institute at the UNC School of Medicine.
Scientists have developed various methods over the past 15 years to reprogram adult cells to become stem cells, then to induce those stem cells to become a different type of adult cell. More recently, scientists have been finding ways to do this reprogramming more directly—directly from one type of mature cell to another. It was hoped that if these methods became as safe, effective and efficient as possible, doctors would be able to reprogram harmful cells into useful ones with the help of simple injections in patients.
“Fibroblast reprogramming has long been one of the important tasks in this field,” Tian said. “Fibroblast overactivity underlies many serious diseases and conditions, including heart failure, chronic obstructive pulmonary diseasediseases of the liver, kidneys and cicatricial lesions of the brain that occur after strokes.’
In the new study, Tian’s team, including co-authors Haofei Wang, Ph.D., Ph.D., and M.D./Ph.D. student Benjamin Kipers used three existing methods to reprogram mouse fibroblasts into cardiomyocytes, liver cells and neurons. Their goal was to catalog and compare the changes in cellular gene activity patterns and gene activity regulatory factors during these three different reprogrammings.
Unexpectedly, the researchers found that reprogramming fibroblasts into neurons activated a set of cardiomyocyte genes. They soon determined that this activation was due to Ascl1, one of the master programmer “transcription factor” proteins used to create neurons.
Because Ascl1 activated cardiomyocyte genes, the researchers added it to a cocktail of three transcription factors they used to make cardiomyocytes to see what would happen. They were surprised to find that it dramatically increased the effectiveness of reprogramming – the proportion of those successfully reprogrammed cells– more than ten times. In fact, they found that they could now drop two of the three factors from their original cocktail, keeping only Ascl1 and another transcription factor called Mef2c.
In further experiments, they found evidence that Ascl1 by itself activates genes in neurons and cardiomyocytes, but that it deviates from the proneuron role when accompanied by Mef2c. In synergy with Mef2c, Ascl1 turns on a wide array of cardiomyocyte genes.
“Ascl1 and Mef2c work together to exert procardiomyocyte effects that neither factor exerts alone, creating a powerful reprogramming cocktail,” Tian said.
The results show that the main transcription factors used in direct cell reprogramming are not necessarily specific to only one target cell type.
Perhaps more importantly, they represent another step toward future cell reprogramming therapies for underlying disorders. Tian says she and her team hope to create a synthetic two-in-one protein that contains the effective bits of Ascl1 and Mef2c and can be injected into diseased hearts to fix them.
Haofei Wang et al. Cross-lineage potential of Ascl1 revealed by comparison of different reprogramming regulators, Cellular stem cell (2022). DOI: 10.1016/j.stem.2022.09.006
Citation: Scientists Discover Protein Partners That Can Heal Heart Muscle (October 6, 2022) Retrieved October 6, 2022, from https://medicalxpress.com/news/2022-10-scientists-protein-partners-heart-muscle.html
This document is subject to copyright. Except in good faith for the purpose of private study or research, no part may be reproduced without written permission. The content is provided for informational purposes only.