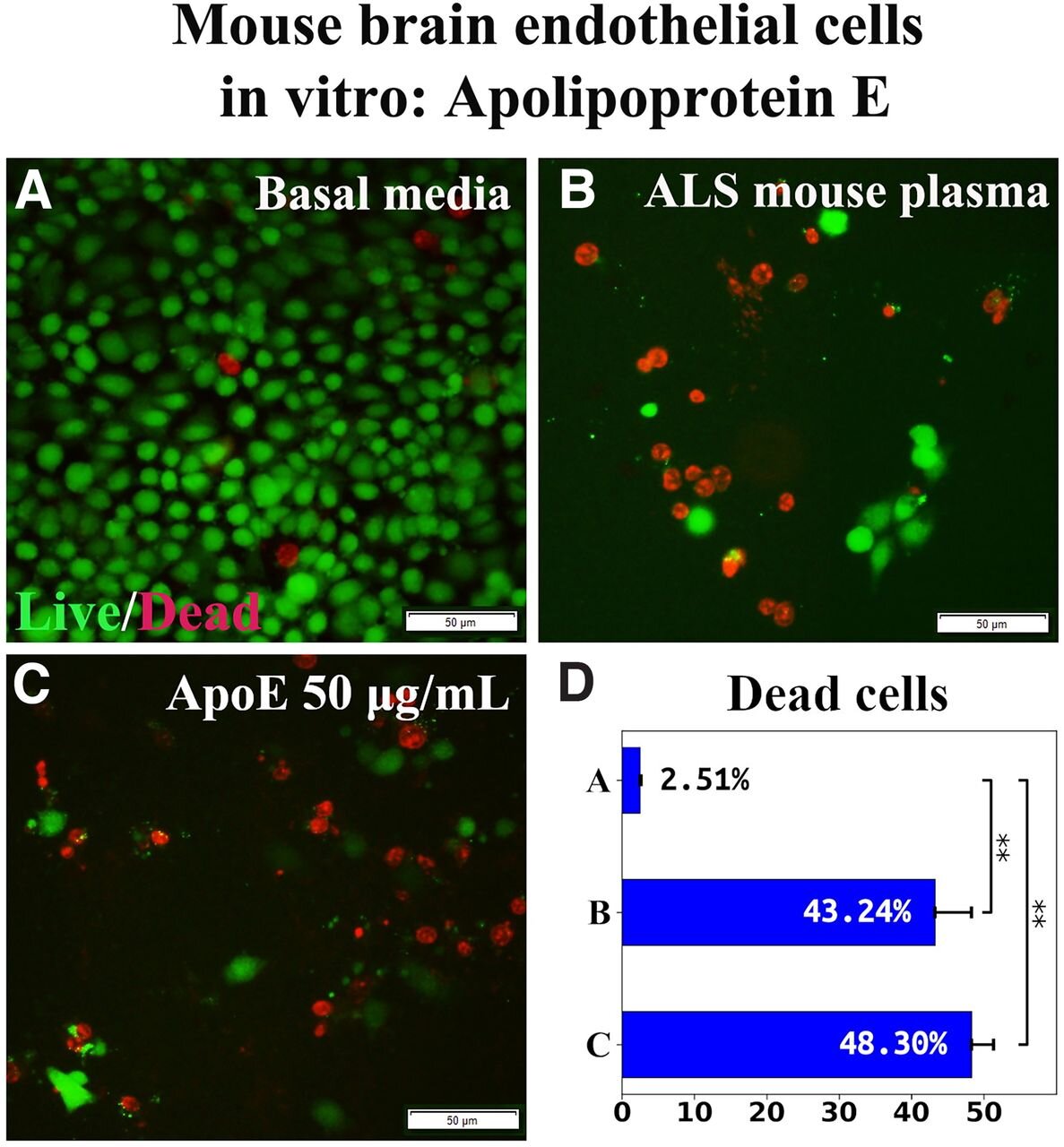
Effect of ApoE on mBEC viability after exposure to plasma from ALS mice in vitro. A, Numerous viable (green) mBECs were observed in cultures with basal media. B, Dead (red) cells increased significantly after exposure to 3% ALS mouse plasma. C, Addition of 50 μg/ml ApoE to culture medium with ALS plasma did not reduce dead cells. Scale bar: 50 μm (AC). D, statistical analysis of display images; **p <0.01. credit: eNeuro (2022). DOI: 10.1523/ENEURO.0140-22.2022
Researchers at the USF Health Morsani College of Medicine at the University of South Florida have successfully tested a protein that could help develop protein therapies for patients with ALS, a progressive disease of the nervous system, also known as Lou Gehrig’s disease, that affects nerve cells in the brain and spinal cord .
Published in eNeuroresearch examines the effect of apolipoprotein A1, “good cholesterol” on endothelial cellslining st blood vessel which provides a barrier between the tissues of the brain, spinal cord and blood circulation.
U petri dish under environmental conditions reminiscent of ALS, the team found that the protein activates a unique pathway in cells that increases survival and protects endothelial cells from toxic substances in the blood. This pathway may enhance cell survival and prevent further vascular damage in ALS.
“With a functional barrier, the hope is that the environment in the central nervous system will become less toxic and disease progression you can slow down,” said Sviatlana Garbuzova-Davis, a professor in the Department of Neurosurgery and Brain Rehabilitation and lead researcher.
Although the protein has been shown to protect endothelial cells in diseases such as diabetes and atherosclerosis, the effect on ALS-damaged endothelial cells was previously unknown.
To test the effect on ALS, the team studied how the protein affects endothelial cell signaling. Garbuzova-Davis and other researchers, USF Professor Alison Wheeling and USF University Professor Emeritus Cesario Borlongan, found that the damaged cells took up the protein, significantly reducing the damage to the endothelial cells.
“It’s too early to predict what the ultimate effect will be for patients,” Willing said. “In this study, we used a cell culture model where we can control all aspects of the exposure of the cells. It is impossible to have the same degree of control in humans.’
Garbuzova-Davis says this study laid the groundwork for additional studies in animal models of ALS to fully determine the therapeutic effect of the protein. If successful, apolipoprotein A1 may be considered clinical trialswhere it will be evaluated for safety and efficacy in ALS patients.
In the near future, apolipoprotein A1 may be considered as a potential new therapeutic agent for endothelial cell repair, restoration central nervous system barrier in ALS patients. It can also help relieve symptoms of ALS, such as imbalanced antioxidant levels and inflammation.
Svetlana Garbuzova-Davis and others. Apolipoprotein A1 increases endothelial cell survival in an in vitro model of ALS, eNeuro (2022). DOI: 10.1523/ENEURO.0140-22.2022
Provided
University of South Florida
Citation: Researchers advance efforts to develop protein-based therapy for people with ALS (2022, October 4) retrieved October 4, 2022 from https://medicalxpress.com/news/2022-10-advance-efforts-protein- based-treatment- therapy.html
This document is subject to copyright. Except in good faith for the purpose of private study or research, no part may be reproduced without written permission. The content is provided for informational purposes only.